Conditions treated

Back Pain
Back pain is a very common complaint, affecting most of us at some stage during our lifetime. Triggers can include sprains and strains, changes in our loading patterns and even inactivity, poor sleeping patterns and high levels of stress.
Although the cause of most peoples’ back pain is not serious pathology, it is important that a thorough evaluation is conducted to exclude the presence of these factors. At ProHealth physio we conduct thorough evaluations to firstly screen for anything serious and then to identify the key factors around the cause your back pain and strategies to help you return to normal as soon as possible.
What we know about back pain
- Back pain doesn’t get worse with age.
- Back pain can be one of the biggest causes of disability
- In most cases back pain is NOT due to any significant structural damage or disease.
- Back pain is usually caused by a combination of things such as:
- deconditioning, changes in activity levels, poor sleep, stress and tension, feeling run down, low mood, inactivity and poor conditioning. Any of these factors may combine to make your back feel very sensitive to movement and load
- Backs love movement and activity, and carrying more load makes backs stronger.
How can we help you
- Give you a clear diagnosis about what are the main factors affecting your back pain.
- Give you a plan to help you control your pain. This might involve hands on work, but always an active management plan.
- We have expertise in the science of back pain, the science of exercise and how to set up an effective management plan
- Take you on a journey to get living again – we will help you achieve your goals!
Back pain MYTHS
- There are a number of myths around back pain which we believe are not helpful (Australian Physiotherapy Association 2020)
- Back pain is inevitable with age
- Backs wear out with everyday bending and lifting
- A weak core causes back pain
- A scan will show me the cause of my back pain
- Pain when exercising means it’s getting worse
- Flareups or pain for a long time means there’s serious damage
- Poor posture causes back pain
- Injections, surgery or strong painkillers will cure my back pain
The good news is that you can take control back of your back pain. If you need help to get moving and Get back to normal, we can help you here at pro health.
Serious causes of back pain
- recent changes to your bladder or bowel habits associated with progressive back and leg pain and loss of power and sensation in the leg
- a history of significant trauma such as a fall from a height such as a ladder or a roof
- a previous history of cancer, feel generally unwell, have significant night pain, a recent history of weight loss

Sports injuries
Our team of physiotherapists have extensive experience working with individuals and elite sporting organisations over many years. We understand the importance of returning to sports as quickly as possible and the frustrations of being injured. The range of sports injuries that we see in the clinic is wide and varied, from Sprained joints such as ankles and shoulders, to Muscle strains such as hamstrings and calves. We will help diagnose and rehabilitate your sports injury with care and dedication to ensure that you make it safe and speedy return to activity. Occasionally if Your injury is more serious in nature, we have a wide range of connections both locally and nationally should your injury require further investigation and further treatment, such as an orthopaedic surgeon or Specialist sports medicine doctor.
We use a wide variety of treatments such as targeted exercise, manual therapy and massage to help you to return to your chosen sport. We can also discuss with your coaches about:
- Modifications to training programmes,
- Gym programmes
- Running programs
- Pitch based returned to play drills.
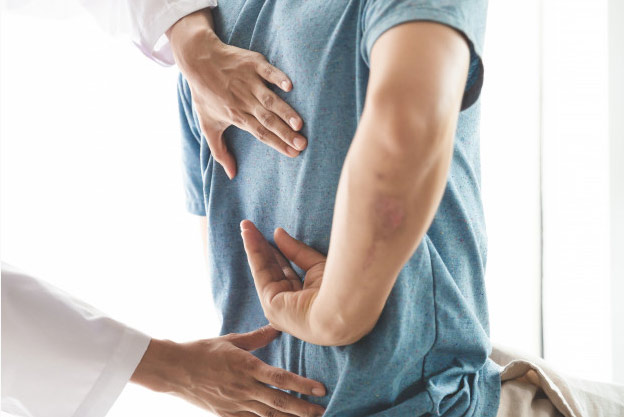
Persistent Pain Disorders
Pain, in particular low back pain, is the leading cause of disability worldwide. The understanding of the complexity of a person’s experience of pain amongst health care practitioners has improved significantly in the last number of years. Our specialist physiotherapists are up-to-date with the most current research and concepts in relation to pain studies and their expertise will enable you to understand your pain experience and help you on the path to recovery. We can confidently help patients with long-term pain issues and those that have seen other practitioners without success.
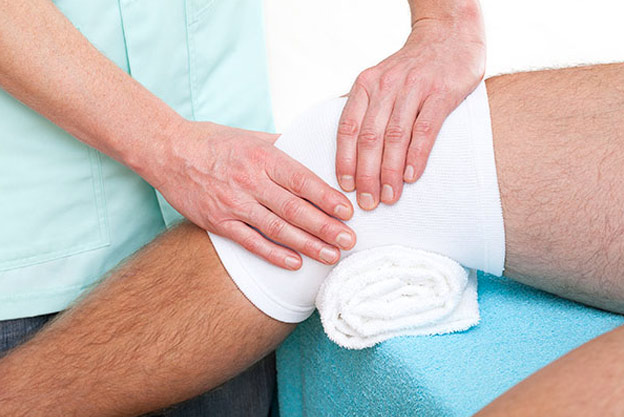
Joint Replacement
Joint Replacement surgery such as hip, knee or shoulder replacement are being undertaken with increased regularity. To optimise your recovery following surgery, our team of specialist physiotherapists will help design and implement a rehabilitation programme for you to help gain mobility, restore range of motion and increase muscle strength which will help you achieve your full potential following surgery.
Stabilisation surgery, such as ACL repair and rotator cuff repairs of the shoulder are also common conditions seen within our clinic. We work closely with the orthopaedic surgeons to ensure the best possible outcome for our clients from the early stages following surgery right up to end-stage rehabilitation and return to sports or recreational activities.
We are also happy to advise on exercise programmes that can be done before you go in for your joint replacement surgery. The benefits of these programmes can include:
- Improving strength of the muscles around the involved joint
- Improving flexibility of the muscles
- Improving cardiovascular fitness
- Improving balance
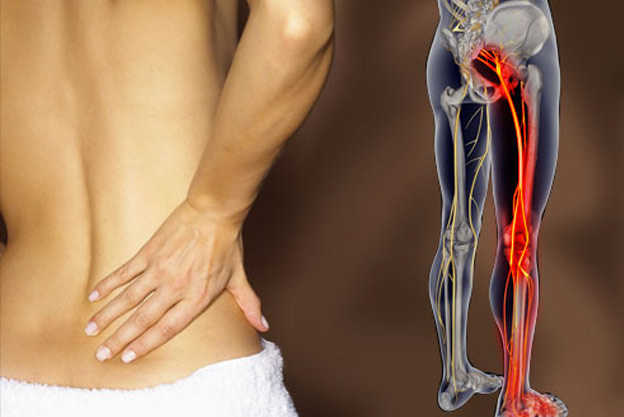
Sciatica
Pain radiating from the back and into the leg is often referred to as Sciatica and can be extremely unpleasant and disabling. Thankfully the symptoms often settle over time and can be helped by a thorough assessment by a skilled physiotherapist who can give you management strategies that will help settle your pain. We also have strong links with other medical professionals should they be required to help.
Pain is usually associated with inflammation around one of the nerves that run down into your leg and can occur with or without compression of the nerve. We will undertake a thorough examination and test for nerve compression including testing reflexes, muscle strength and sensation. In the unusual event of bladder/bowel changes and a progressive worsening of compression symptoms, urgent medical review is needed.
In most cases natural recovery is very good over 8-12 weeks with the most symptoms resolved by this time. Our physiotherapists can provide you with a thorough assessment and a management program to help you return to normal as quickly as possible.

Shoulder Pain
Shoulder pain is very common. It is estimated that 3 in 10 adults are affected by shoulder pain at some time. Shoulder pain can be a long-term problem. Up to half of people can have symptoms after 18 months. Therefore, it is important to get the correct diagnosis so that you can receive effective treatment for your symptoms.
Shoulder pain can be caused by several different conditions such as frozen shoulder, rotator cuff disorders, shoulder instability and acromioclavicular joint disorders. Exercise is the most effective treatment plans for shoulder pain.
Facts
- Shoulder pain is common without any significant structural damage to the joint.
- Lots of people WITHOUT shoulder pain have rotator cuff tears.
- Rotator cuff tears do not predict shoulder pain.
- Noisy shoulders are common and not a sign of damage.
- Scans are usually only needed if you have had a traumatic injury.
- Using your arm and getting it stronger reduces your shoulder pain.
- Lifestyle factors such as diet, sleep and general health are all important for relief of shoulder pain.
- Cortisone may offer short term relief, but you need a long term rehab program to get your shoulder back on track.
Myths
- Shoulder pain is a sign that I’ve seriously damaged or torn something.
- A noisy or clicking shoulder is a sign that there must be something seriously wrong.
- An MRI is needed to see what is wrong with my shoulder
- I should rest my shoulder.
- All I need to fix my shoulder is a Cortisone injection
- If I’ve torn my rotator cuff tear I must need surgery
How can ProHealth Physiotherapy help you?
- Diagnose the cause of your shoulder pain and determine whether further investigation is needed.
- For people who have had shoulder pain for a long time we have a lot of experience in assessing and identifying the important factors affecting your pain and making a plan to get you back to your valued activities.

Knee Pain
Knee pain is a term given to pain around the front, back and side of the knee. Pain around the knee can be related to tendons, muscles, the knee-cap or the knee joint itself. Knee pain usually presents during loading such as standing, walking, running, walking downstairs, squatting and can disrupt sleep. Exercise has been shown to be just as or more effective than surgery for conditions such as osteoarthritis of the knee.
Helpful Advice
- Exercises such as squatting, step-ups and walking help strengthen to the knee
- Lifestyle factors such as diet, sleep and general health can improve knee pain
- Increase physical activity from a distance and pace which is comfortable for you and increase your activity as your pain allows.
Unhelpful Messages
- Stop exercising if the knee is painful
- Rest until knee pain goes away
- Avoiding weight bearing exercises such as step ups, running, jumping or squatting
- Getting a scan to find source of knee pain
- Look for surgical intervention or injections as first line of treatment
How can ProHealth Physiotherapy help you?
- We can diagnose the cause of your pain and develop a plan to manage your symptoms
- If you have developed pain over a long period of time, we will help you identify the key factors related to it
- We have close working relationships with a network of Orthopaedic Surgeons, Sports Medicine Specialists, as well as GPs, should the need arise for further investigation or treatment.

Arthritis
Arthritis is a description for changes to your joints and may be associated with pain swelling and stiffness. The most common types of arthritis are osteoarthritis (OA) and rheumatoid arthritis (RA). Osteoarthritis causes changes in the cartilage of our joints. Rheumatoid arthritis is a disease in which the immune system attacks the joints, beginning with the lining of joints. Other types of arthritis can result from gout, infections or disease, such as psoriasis or lupus. Treatments vary depending on the type of arthritis but the main goals of physiotherapy for arthritis is to reduce symptoms and improve quality of life.
The Facts About Arthritis
- An X-Ray is not a good indication of how sore your joints are
- The amount of arthritic change on a scan is a poor predictor of pain and disability
- Abdominal fat, muscle weakness, protective muscle guarding, and lack of confidence of using the joint is a predictor of pain and disability
- Building up the strength of the of muscles around the arthritic joint can help to reduce pain
- Getting fit, strong and normalising the way you move, can help to reduce pain and disability
- A 10% reduction of body weight can lead to a 50% reduction in pain
UNHELPFUL THINGS people say about Arthritis
- Arthritic joints always need surgery.
- Arthritic joints always cause pain and disability.
- Exercise for arthritic joints makes them worse.
- People with arthritic joints need to rest.
How can ProHealth Physiotherapy help you?
- We can identify the key factors linked to your pain
- We can set you up with a specific rehab plan to get you strong, relaxed and confident
- We work with other health professionals to assist with weight loss

Headaches
There are many different types of headache, such as migraine, tension headache, cluster headache and neck-related headache.
There can be a number of different causes of headache, most of which are not serious, however occasionally headache can be a symptom of a more significant underlying disorder. In these cases, a medical review should be sought immediately. A detailed examination by one of our skilled physiotherapists can help to determine the type of headache you may have and provide you with a plan to get you back to normal. A combination of exercise, ergonomic changes, recognising aggravating factors can all be part of the management of headaches.
What we do know about headaches
- There are three main types of headache:
- migraine
- tension headache
- headache from the upper neck
- Inactivity, ergonomic factors, poor sleep patterns, stress, worry and low mood can all be associated with headache
- Working with a qualified physiotherapist can help with tension and neck related headaches
Headaches are NOT caused by
- neck being ‘out’
- by poor posture
- by weak muscles
How can PROHEALTH Physiotherapy help you?
- Diagnose the type of headache you have.
- Provide exercises, relaxation, ergonomic advice and stress management strategies for tension headaches
- Use exercise, advice and some hands-on techniques, we can help reduce the pain caused by neck-related headaches
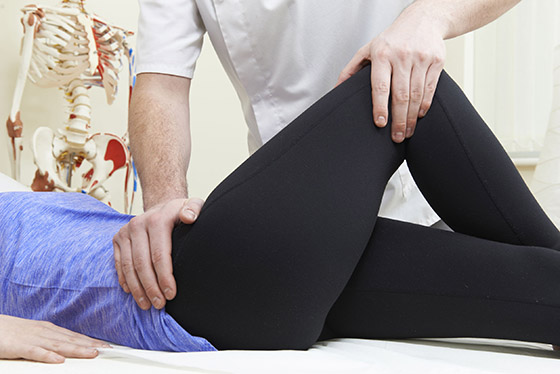
Hip Pain
Hip pain is any pain around the buttock, outside the hip and or the groin. It can sometimes move down the leg and could also be associated with back pain. Hip pain can be related to the tendons, muscles or hip joint itself.
Common complaints that may cause hip pain include gluteal tendinopathy, labral tears, trochanteric bursitis and hip arthritis. Hip pain usually presents with pain when loading the hip such as walking, running, standing and is commonly aggravated while sleeping especially when lying on the side.
Some Facts about
- A noisy or clicking hip DOES NOT mean your hip is damaged.
- Pain coming from the hip joint is hard to locate and is usually felt into you groin and top of the thigh
- Exercise has been shown to help reduce hip related pain
- A big part of long-term hip pain can be because of muscle changes and protective movements causing irritation by increasing compression of the joint
- The stronger your hip muscles are the more they can help with absorbing shock when you are loading your hip.
- The pain in your hip and what is on an MRI scan DO NOT always match.
- People can make a full recovery back to everyday function and elite level sport after hip injuries.
Unhelpful ideas about HIP pain
- A hip injury could end my career
- Pain at my hip means I have seriously damaged something.
- My hip pain has been there for years so it must be arthritis.
- If exercise hurts my hip, I need stop it.
- I’m too young to have hip pain.
- Noises around my hip must be causing problems
- If I just ignore my pain it will probably go away.
How can Pro Health Physiotherapy help with your HIP pain?
- Use the most up to date assessment techniques and strategies to correctly diagnose the cause of your hip pain
- We can provide a return to running or gym-based exercise programme.
- Give you evidence-based advice about whether you need a scan or not.
- In most cases we will take you through 3 stages of rehab
- Settling the pain with advice and gentle exercise and hands on treatment if needed
- Getting strong with progressive specific exercise rehabilitation
- A return to play program for sports
- We can link with a surgeon/ sports consultant regarding assessment and rehabilitation.

Neck Pain
Neck pain is a common problem that affects many people at some time in their lives. Neck pain can involve the neck and shoulders, or it may radiate down an arm. The pain can be dull or feel like an electric shock into your arm.
Physiotherapy can help diagnose the source of your pain and help you manage it. Certain other signs and symptoms, such as numbness or muscle weakness in an arm, can help pinpoint the cause of your neck pain.
Facts
- Neck pain is rarely caused by significant damage to bones or discs
- Neck pain may be linked to factors such as stress, muscle tension, a strain, poor sleep and activity levels.
- Getting fit, strong and normalising the way you move helps neck pain.
- So-called abnormal findings on scans like disc bulges and degeneration are common in most necks without experiencing pain.
Unhelpful ideas
- Turning or twisting your neck is dangerous when your neck is sore
- If your neck is sore there must be something out of place
- Bad posture is causing your neck pain
How can ProHealth Physiotherapy help you?
- We can identify the keys factors linked to your neck pain.
- We can help relieve your pain, reduce muscle tension and get you moving again.
- We can set you up with a specific rehab plan to get you strong, relaxed and confident.
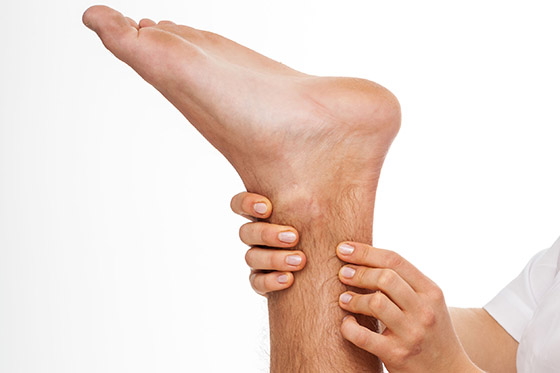
Tendon Pain
Tendon pain, also referred as tendinopathy is when the structure of the tendon is disturbed by repetitive strain, causing inflammation. This cumulative microtrauma weakens the tendon, which ultimately leads to tendinopathy, especially if recovery is not allowed. These injuries can be very painful and prevent participation in sports and other recreational activities. Common sites where we experience tendon pain are:
- Achilles (behind the ankle)
- Patellar (front of the knee)
- Rotator cuff (shoulder)
- Tennis elbow (outside of the elbow)
- Golfers elbow (inside of the elbow)
This can happen when there is excessive load placed on the tendon too quickly, for example if someone starts running and increases their mileage.
Facts
- Tendons don’t like sudden increases in load.
- Tendons adapt to graduated loading.
- Strengthening the muscles around the tendon helps.
- Loading a painful tendon is not dangerous – it won’t snap.
- Painful tendons get better with the right treatment.
Myths
- Tendons need to be rested, massaged and stretching.
- Tendon injuries always need surgery.
- The amount to pain always reflects the amount of damage done.
How can ProHealth Physiotherapy help you?
- We can set you up with a specific rehab plan to gradually get you loading your tendon and strengthen your muscles to get you back to normal sports and recreation activities.

Joint Laxity / Instability
Joint laxity and hypermobility is common and there is a great deal of research to suggest that it does not cause long term pain or damage to joints. Exercise is helpful and can help provide support and control to joints that have more movement than is usual. Dancing and gymnastics can be beneficial for hypermobility/joint laxity.

Whiplash
Whiplash is a neck injury due to forceful, rapid back-and-forth movement of the neck. Whiplash most often occurs during a rear-end road traffic accident, but the injury can also result from a sports accident or other trauma. Whiplash is quite common and can be sore, scary and give you stiffness and headaches for some time. Most people with whiplash get better within a few weeks with some good advice, exercise and maybe some pain medication.
Facts
- Whiplash can be scary and painful – but it rarely results in long term damage to the neck structures.
- Whiplash is associated with a strain to the soft tissues (ie muscles and ligaments) that get better with the right treatment.
- Resting, worrying, protecting the neck, and avoiding movement are the worst things to do following whiplash.
- Too much treatment can make things worse.
Myths
- Whiplash means your neck is seriously damaged.
- You need to rest and avoid moving to let your neck heal.
- Whiplash needs a lot of treatment.
How can ProHealth Physiotherapy help you?
- We can provide you with strategies to relax your neck, be confident, get strong, and moving normally again.
- We can help get you back to enjoying life as quickly as possible.
- We don’t over treat whiplash – we know it doesn’t help.

Plantar Fasciitis
Plantar fasciitis is a common causes of heel/foot pain. The pain usually involves inflammation of a thick band of tissue that runs across the bottom of your foot and connects your heel bone to your toes (plantar fascia). Plantar fasciitis commonly causes pain, that usually occurs first thing in the morning. As you get up and move more, the pain normally decreases, but it might return after long periods of standing or after rising from sitting. Plantar fasciitis can be treated effectively with exercise.
Helpful
- Wear comfortable supportive footwear
- Gently move your feet up and down first thing in the morning for 2-3mins before putting your feet on the ground
- Do stretches as prescribed by your physiotherapist at least 2-3 times per day
Unhelpful ideas
- Walking on bare feet even at night to go to the bathroom
- Wearing slippers or sandals
- Avoiding exercise
- Rolling a golf ball or something hard under your foot
How can ProHealth Physiotherapy help you?
- At ProHealth Physiotherapy, we will assess you to determine the reason for your foot pain.
- We will then make a treatment plan designed for your needs so that you can return to your previous activity level as soon as possible
- Orthotics may be required to reduce strain on your foot however, if required this will be discussed with you during your consultation
Pelvic Health
Listening to our clients’ stories over the years & having seen the negative effects that these conditions can have on a person’s quality of life, I am determined and passionate about the importance of educating people, in particular women, about their pelvic health. I firmly believe that a thorough examination at the ante natal stage and definitely at the post-natal stage is essential, as early intervention is key.
The Facts
- In Ireland, 1 million women have some degree of incontinence (1 in 3 women suffer)
- Incontinence can be very embarrassing
- Incontinence doubles risk of post-natal depression (Journal of Obstetrics & Gynaecology in 2011)
- Weak Pelvic floor increases risk of falls (rushing to the loo, distressed)
- Lack of Awareness among Health Care Professionals or women themselves that Specialised Chartered Physios exist to address these issues
We know from research that a thorough assessment & diagnosis with a Pelvic Health physiotherapist and a follow on individualised, evidence-based treatment plan can help to alleviate any symptoms you may be experiencing.
If you are…
- Afraid to go out in case you leak or are tired of wearing incontinence pads;
- Afraid to jump on the trampoline or go running or dancing
- Afraid to move or go for a walk
- Afraid to have sex because you might leak or its too sore
- Tired because your child is wetting the bed
- Anxious about a dragging sensation in your vagina
- Embarrassed about staining your underwear
You are not alone. Whilst these conditions are common, continuing to “put up” with the symptoms is not normal and they are treatable.

Pelvic floor Dysfunction
What is the Pelvic Floor?
What is Pelvic Floor Dysfunction?
Who can it effect?
- Children (bed wetting and constipation)
- Active teenagers usually involved at a high level in Sport
- Athletes (again performing at a high level)
- During pregnancy
- After child birth
- During the menopausal years
- After surgery (abdominal, pelvic, spinal, prostatectomy)
- Prolonged bed rest
- Aging
RISK FACTORS
- Obesity
- Multiple Births
- Weight of baby at birth >8lbs
- Forceps delivery
- Episiotomy during delivery
- Repeated, heavy lifting eg at the gym
- Incorrect toileting habits (particularly learned from childhood)
- Inappropriate exercise: overtraining, incorrect use of weights, incorrect techniques particularly sit ups
- Chronic lung conditions that can bring on prolonged coughing eg asthma, COPD, Cystic Fibrosis
- Any condition that can weaken your pelvic floor muscles such as Multiple Sclerosis
What to Expect at a Pelvic Health Assessment?
With your consent, I will complete a full physical assessment of your problem and this usually involves an internal examination
I will then design an individualised programme to suit your needs
At all times your right to confidentiality and dignity will be respected
Incontinence
Incontinence is a term that describes any accidental loss of urine from the bladder (urine incontinence) or leakage of stool and/ or flatus (wind) from the anus (faecal incontinence). Leakage of urine because in 2 types:
- stress incontinence (when you laugh, cough, sneeze or lift)
- urge incontinence (sudden desire to go to the toilet +/- frequency)
Facts about incontinence
- Incontinence occurs in people of all ages and affects men (1 in 10), women (1 in 3) and children. it can be a great source of embarrassment to those affected
- Wearing pads is not the best solution
- Drinking less fluid does not improve incontinence
- Incontinence doubles the risk of post- natal depression (Journal of obstetrics and gyanecology 2011 )
- Weak pelvic floor increases risk of falls in the elderly (rushing to the toilet)
- Incontinence is one of the major reasons why the elderly are forced to go into a nursing home
- Mild occasional incontinence is often a warning sign to seek help but if left untreated leakage can happen everyday
- You are never too old to seek help
- Lack of awareness among healthcare professionals or women /men themselves that specialized chartered physiotherapists in pelvic health exist to help with these issues
- 1 in 3 of women performed their pelvic floor muscle exercises incorrectly
Incontinence can be caused by pelvic floor dysfunction
Pelvic floor dysfunction is any urinary or faecal incontinence or obstruction, Constipation, vagina or uterine prolapse, vagina or rectal pain, sexual dysfunction or pelvic pain (Mary O’Dwyer 2001)
Pelvic floor dysfunction can affect:
- Children (bed wetting and Constipation)
- Active teenagers usually involved at a high level in sport
- Athletes (again performing at a high level)
- Pregnancy
- After childbirth
- During the menopause
- After surgery (abdominal, pelvic, spinal and prostate)
- Prolonged bed rest
- Aging
Risk factors
- Obesity
- Multiple births
- Weight of baby at birth > 8 pounds
- Forceps delivery
- Episiotomy during delivery
- Repeated heavy lifting
- Incorrect toileting habits (particularly learned from childhood )
- Inappropriate exercise: over training, incorrect use of weights, incorrect techniques particularly with abdominal setups
- Chronic lung conditions that can bring on prolonged coughing such as asthma
- Stress and anxiety with other general health conditions such as irritable bowel syndrome can cause your public floor muscles to become overactive and can lead to difficulty with emptying your bowel and or bladder
Management of incontinence
Pelvic floor exercises are some of the best treatment tools recommended by the international continence society and is the first line treatment before surgery. 83% of women improve!
What to Expect at a Pelvic Health Assessment?
- I will begin by listening to your story and taking a detailed history
- With your consent, I will complete a full physical assessment of your problem and this usually involves an internal examination
- I will then design an individualised programme to suit your needs
- At all times your right to confidentiality and dignity will be respected

ACL Injury
An ACL injury is a tear or sprain of the anterior cruciate ligament (ACL) — one of the major ligaments in your knee. ACL injuries most commonly occur during sports that involve sudden stops or changes in direction, jumping and landing — such as Galeic football, soccer, rugby, football and hurling.
When an ACL injury happens, people may hear or feel a “pop” in the knee. This often happens without direct contact with an opponent. Your knee may swell, feel unstable and be sore to put weight on however on occasions, people may be able to keep playing.
Depending on the type of ACL injury you have, treatment may include rest and rehabilitation exercises to help you regain strength and stability or surgery to replace the torn ligament. Surgery is always followed by rehabilitation. An evidence-based training program is an essential part of recovery and may help reduce the risk of a recurrence of an ACL injury.
We have extensive experience In the assessment And management of ACL injuries with many years of working with elite sports teams and amateur athletes. we have helped many amateur and professional sportsmen and women with their rehabilitation back to their chosen sports. ACL injuries can be accurately diagnosed clinically however assessment often includes MRI and opinions from orthopaedic surgeons. We can advise on this and make referrals to appropriate medical practitioners.
Incorrect or Unhelpful Ideas that don’t help:
- Rehab doesn’t make a difference with ACL recovery
- Rehab shouldn’t start until one month after surgery
- All ACL injuries require surgery.
- Recovery from ACL surgery and return to sport takes a minimum of 12 months.
BEST Evidence and Practice
- If you have an ACL tear, your confidence in your knee is one of the best predictor of outcome.
- Some people with an ACL rupture don’t require surgery if they are rehabilitated well.
- Returning to sport is based on your strength, agility, function, and type of graft (if you’ve had surgery).
- Resting your knee for too long will reduce your muscle strength and delay your recovery.
How will ProHealth Physiotherapy help you with your ACL ?
- We can help with a quick diagnosis of your knee injury.
- We can develop an exercise program that is specific to YOU.
- We will give you the most up to date advice and best rehabilitation evidence to help your recovery
- We have close relationships with many orthopaedic surgeons and we will communicate with your surgeon to work out the best time frame for your return to sport
- We will perform specific return to sport tests, designed around your sport and your needs. We will make sure you are safe and confident before getting back to competition.
Nerve Pain
Nerve pain is often caused by inflammation rather than compression of a nerve and surgery is rarely needed. We can assess the dominant type of pain you are experiencing and how to optimize the environment whereby the nerve can heal. By understanding the main drivers of your pain it is possible to get moving and active.
The natural pattern of resolution of inflammation is normally 8-12 weeks and symptoms normally resolve over this period. following a thorough examination, we can advise on strategies that will help you get back to normal as soon as possible. We can communicate with other medical professionals that can help if necessary, such as GP’s and other pain management disciplines.
We will also discuss with you possible risk factors for development of nerve pain strategies that can be employed 2 reduce the risk of subsequent bouts of nerve pain. These may include:
- exercise programmes
- Weight management strategies
- Sleep and lifestyle advise
See sciatic pain.
